Early
Covid-19
treatment
Guidelines.
A Practical Approach to Home-based Care for Healthy Families
This is an up-to-date guide to managing Covid-19 illness effectively at home. Covid should be treated early, with a combination of therapies, and treated aggressively to avoid the more dire consequences of the illness, although most cases now seem to involve mild variants like Omicron that range between cold-like symptoms to flu-like symptoms depending on your age, immune response, and general health.
This Covid-19 treatment guide is informed by both established and emerging medical research as well as the clinical experience of international doctor-led groups; it will evolve as new evidence emerges.
The safe, established, and patent-free medicines and supplements included in this guide may have differing availability around the world. For that reason, a variety of medicines have been included. Expensive, new drugs (such as monoclonal antibody treatments) are not considered here, although they can be accessed in the USA and certain other countries.
We envision a world where you are empowered to take control of your health. This resource is a living guideline and will change as new evidence emerges. It does not provide individual medical advice or prescribe treatment.
The guide is intended to empower individuals and their families with knowledge of healthcare options that may be beneficial to them. Readers should consult the health professional(s) of their choice for individual medical evaluation and recommendations for treatment tailored to their individual needs. This guidance will evolve as new information emerges, so please sign up for email updates to keep abreast of the latest developments.


This is an up-to-date guide to managing Covid-19 illness effectively at home. Covid should be treated early.
Anyone can get Covid-19, whether they have had a Covid-19 injection or not. The good news is that the illness is easily treated, and most people will recover within a few days or weeks.

By treating your illness early, you will be helping to end the Covid-19 pandemic.
If you or a family member have had a positive test and have symptoms suggestive of Covid-19, this is a practical guide to help you recover quickly. This guide is designed for those who are generally healthy and not taking other daily medications to empower you to beat Covid-19 and get healthy again as quickly as possible.
This document does not apply to pregnant women, who can find useful Covid-19 guidance here.
In this guide, we will answer the questions:
What are the symptoms of Covid-19?
What can I do to treat mild Covid-19 at home?
How does the illness progress?
When should you go to the hospital with Covid-19?
We envision a world where you are empowered to take control of your health. This resource is a living guideline and will change as new evidence emerges. It does not provide individual medical advice or prescribe treatment. Rather, it is intended as a resource to empower individuals and their families with knowledge of healthcare options that may be beneficial to them. Readers should consult the health professional(s) of their choice for individual medical evaluation and recommendations for treatment tailored to their individual needs.
The first thing you should do is tell your family and doctor. Stay home, rest, drink lots of antiviral and anti-inflammatory infusions with freshly chopped ginger and splintered cinnamon sticks with a little good-quality honey and follow the at-home guidance below.
Early treatment will prevent disease progression. cile ci-dessous.
Un traitement précoce empêchera la progression de la maladie.
What are the symptoms of Covid-19?
The Covid-19 pandemic appears to be the result of a virus called the SARS-CoV-2 virus. It has three overlapping phases:
The viral phase (day 1-5)
The inflammation phase (day 1-10)
The hyper-inflammation phase (up to 30 days)
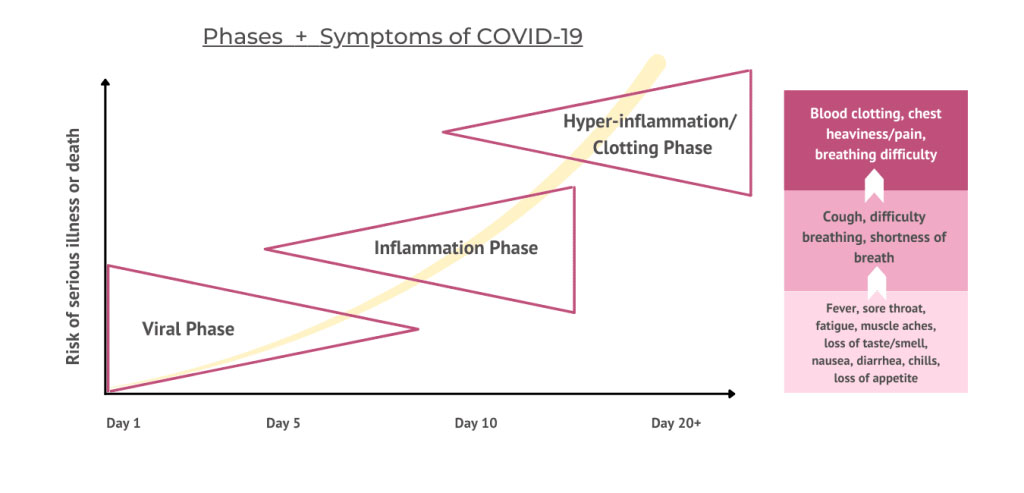
Early symptoms of the virus during the viral and inflammation phase can be any combination of the following:
Fever or chills
Sore throat
Coughs & sneezes
Congestion or runny nose
Shortness of breath or difficulty breathing
Constriction or pressure in the chest area
Mild to extreme fatigue
Headache
Loss of taste or smell
Nausea or vomiting
Diarrhoea
The Inflammation Phase (Day 6 – 10)
During the viral phase of the illness, the SARS-CoV-2 virus replicates rapidly in the body unless you take quick action, just like with a cold or flu or other respiratory or gastric viral infections.
Someone in the viral phase of the illness can expect flu-like symptoms such as fever, joint and muscle pain, headache, sore throat, loss of appetite, loss of taste/smell, nausea, diarrhea, and weakness.
Transmission is highest during the viral phase of the illness, so avoid contact with people during this phase of the illness. It is important to note that asymptomatic people (those who test positive without symptoms) are unlikely to transmit the virus.
During the inflammation phase, your body’s immune system response has geared up to fight the infection and then there is production of excessive amounts of cytokines, which are signalling molecules, proteins used by the immune system to drive its response. When there are too many of them, this can damage the tissues and organs of the body, like with inflammatory and autoimmune diseases.
A person in the inflammation phase of Covid-19 may continue to experience flu-like symptoms, which with underlying pre-existing inflammation, may progress to excess inflammation in lung cells leading to feelings of breathlessness, coughing, difficulty breathing and possibly a secondary bacterial infection like pneumonia. If you are clearly having difficulty breathing, you should follow your doctor’s advice and go to the hospital if he or she cannot attend to you at home.

This graphic represents a general overview of treatment essentials and categories. Most essential medicines and therapies fall into more than one category. Early treatment is key – a combination of therapy approaches is ideal. For a longer list of options, refer to the Summary of Medicines table at the end of this PDF.
*Use acetaminophen / paracetamol sparingly because it reduces glutathione, an important antioxidant
Having a thermometer at home is useful to check whether you have a fever. A temperature over 37.5°C that makes a person feel unwell can be treated with acetaminophen (paracetamol) if the fever continues for longer than is necessary for the immune system to naturally clear the infection.
A nebuliser is a device that turns a solution into a mist, which then gets inhaled through a mouthpiece. It can be useful to deliver solutions such as saline to help with phlegm. Some international doctors also suggest nebulised colloidal silver, which has antiviral properties, nebuliser iodine solution, iodine with salt pipe inhalers, ozone treatment, sodium bicarbonate solutions and chlorine dioxide solutions for Covid-19.
A pulse oximeter is a small piece of equipment clipped onto a finger to measure the oxygen saturation of the blood. It is non-invasive and, in the context of Covid-19 illness, the test results determine whether a person needs to receive additional oxygen and therefore equip the home or, if unavailable for home treatment, be admitted to hospital. If you have access to a pulse oximeter, a reading of 94% or less indicates you are not getting enough oxygen. This waxes and wanes so, in the event, a home oxygen tank can be obtained depending on where you live and whether your chosen health professional will prescribe or order it for you.
Over the course of the coronavirus outbreak, much has been learned by doctors and scientists around the world, and we now know how to treat Covid-19 at home. With early treatment, the risk of more serious disease goes down dramatically, especially with recent Omicron variants.
It’s a good idea to be prepared with simple medicines and therapies in your home dispensary as you would for the cold and flu season before you or your family members get sick.
The spike protein is a major component of the virus. It is toxic and affects the body in several different ways which is why it’s important to use a combination of the therapies to fight coronavirus disease.
Infected individuals should use a combination of therapies that:
Early Covid-19 Treatment Guidelines_V7FH_ENGLISH
Target the virus (antivirals/antimicrobials)
Reduce inflammation in the body (anti-inflammatories)
Support the immune system
Reduce the risk of blood clots (anticoagulants)
Provide symptomatic relief for headaches, fever, cough, etc.
Most recommended therapies and medicines play more than one of these roles to combat Covid-19. Depending on availability in your area, prepare to treat with an agent in each of these five categories to maximize the chance of a speedy recovery.
Ivermectin has antiviral, anti-inflammatory, and immune-supportive properties. This means that ivermectin can be used in all phases of COVID illness, from early asymptomatic infection to more severe illness, including for hospitalized Covid-19 patients.
For early treatment of SARS-CoV-2 infection at home, the recommended dose is 0.4 – 0.6mg per kilogram of body weight per day for five days. In addition to being influenced by body weight, dosing might also be affected by the severity of the coronavirus infection and the virulence of the variant.
Ivermectin
Ivermectin is widely used as an anti-parasitic medicine and, as such, is available in many countries over-the-counter (OTC). It comes in 3mg, 6mg, and 12mg tablets. A liquid suspension may also be available in some countries.
For non-hospitalized adults of average body weight (between 50 to 80kgs), the dose of ivermectin is two to four 12mg tablets daily with food for five days. Longer treatment or higher doses may be necessary, but this should be discussed with a doctor.
Side effects include nausea, diarrhea, dizziness, and rash. These tend to be mild and usually resolve upon discontinuation. Ivermectin is not recommended for use in children under 5 or pregnant women (particularly in the first trimester) without the advice of a doctor.
If you take blood-thinning medication, please consult a doctor before taking ivermectin as ivermectin also has blood-thinning properties.
Because so much virus is in your mouth and nasal passages, it is useful to rinse them several times a day with a sodium bicarbonate mixture, or a saline solution made with warm water and sea salt.
Gargling regularly with propolis extract in warm water or applying it to the back of the throat is also very efficient at preventing viral replication.
Rinsing can also provide symptom support for those with excess mucus and phlegm.

Doxycycline
Doxycycline is an antimicrobial drug commonly used to treat acne and Lyme Disease and prevent malaria. As it also has potent antiviral properties, many
Covid care experts use doxycycline (100mg every 12 hours for 7 days) and ivermectin together in early infection.
Hydroxychloroquine
Hydroxychloroquine is a widely used anti-malarial drug. Its antiviral properties make it a useful alternative to ivermectin in the early treatment of Covid-19 at standard doses (200mg every 12 hours for 7 days). In settings with more virulent Covid strains (e.g., Brazil), Covid care experts sometimes use hydroxychloroquine and ivermectin together, along with zinc and a macrolide antibiotic like azithromycin.
Antibiotics (for symptoms related to lungs and secondary bacterial infection)
If you develop chest symptoms, your doctor may need to prescribe you an antibiotic to prevent or treat suspected pneumonia, like azithromycin with zinc.
2.
Anti-inflammatory medical drugs include prescription steroids (e.g., budesonide, prednisone, dexamethasone, methylprednisolone), non-steroidal
anti-inflammatories (e.g., ibuprofen and aspirin), and certain other well-established medicines (e.g., colchicine and ivermectin).
Ibuprofen
Ibuprofen is a non-steroidal anti-inflammatory drug that is used to treat pain by reducing inflammation in the body. It is available for general use in most countries and helps to reduce the inflammation and joint pain associated with Covid-19, and other viral infections.
Antihistamines
Antihistamines are usually used to treat allergies. They work by blocking the action of histamine; a chemical released when you have an allergic reaction. Oral antihistamines such as loratadine and cetirizine, commonly used OTC medicines for hay fever and rash, may help prevent an allergic immune response (mast cell activation) to the spike protein.
N-Acetyl Cysteine and Glutathione
Glutathione is a powerful natural antioxidant that is found in most cells of the body. Its role is to protect cells by neutralizing toxins. Glutathione often becomes depleted during periods of illness.
N-acetyl cysteine is a drug that breaks down toxic substances by replenishing glutathione. N-acetyl cysteine also helps loosen thick mucus in the inflammatory phase of Covid illness. Both are available as supplements.
Curcumin, Astragalus, Ashwagandha, Holy Basil, Liquorice, Rosemary, Uña de Gato (uncaria tomentosa)
There are many different herbs and supplements that have scientifically proven anti- inflammatory effects. If you have a favourite from your part of the world or one you have already heard of, don’t hesitate to get it into your diet as a herb, tincture, supplement, or whatever form you can get.
3.
Many nutritional supplements like Vitamin D, Vitamin C, Zinc, Quercetin, Melatonin, Glutathione, and N-acetyl cysteine have powerful anti-inflammatory, antioxidant, and immune-balancing properties. These therapies are simple, generally safe, and accessible for home-based treatment, and they do not require a prescription.
Vitamin D
Vitamin D plays an important role in immunity. A deficiency in Vitamin D has been correlated with more severe Covid-19 illness. Many people are low on this essential vitamin due to age or lifestyle. Maintaining good levels of this vitamin is critical for Covid-19 prevention and treatment. Oil-based Vitamin D capsules or drops are preferable to the tablet form, but you may use whatever is available and affordable. In many countries doctors will prescribe it in clinical doses when blood test show it is low as it is critical for your immune response. Vitamin D is best absorbed with a meal.
Vitamin D can also be produced by the skin when it is exposed to sunlight, depending on your age, skin colour and latitude. Getting daily sunshine is vital for both the prevention and treatment of Covid-19.
Vitamin C and Zinc
Similarly, Vitamin C and Zinc have antiviral, anti-inflammatory, and antioxidant properties and are used in various viral illnesses, including Covid-19. Vitamin C can be found in many fruits and vegetables, especially citrus fruits. Zinc is available in foods like beef, chicken, and fish but, in the context of Covid infection, you should use supplemental levels of both to ensure adequate levels are achieved, ask your health practitioner for advice on dosing as both decrease dramatically in the event of an infection and they are essential for your immune response.


Quercetin
Quercetin is a plant pigment or flavonoid widely available in fruit and vegetables, most notably parsley, berries, red onions, apples, and citrus fruit. Quercetin can be taken as a supplement to help support the immune system during an infection along with zinc. Like hydroxychloroquine it also transports zinc into your cells, thereby blocking viral replication.
Melatonin
Melatonin is a hormone made in the pineal gland in the brain, which kicks off the sleep cycle in the evening. It is a powerful antioxidant. Studies show that melatonin reduces cytokines (proteins associated with inflammation) and improves sleep quality which is vital during a viral illness. When used as a supplement, melatonin is best taken before bed.
Glutathione
Glutathione is a powerful antioxidant that is found in most cells of the body. Its role is to protect cells by neutralizing toxins. During periods of illness, glutathione often becomes depleted.
Nigella sativa
Nigella sativa, or black cumin seed is a natural substitute for ivermectin when this is not available. This plant extract inhibits viral replication by binding to ACE2 receptors, counters mRNA expression and is anti-inflammatory and analgesic. Attention if taking anticoagulant medication as it is also an anticoagulant.
4.
A dangerous feature of severe Covid-19 is blood clotting. Anticoagulant medications are used to prevent blood clots from forming in the legs, lungs, heart, and other parts of the body.
Aspirin
As a cheap and widely available medicine, daily aspirin is recommended for early Covid-19 infection to prevent this serious complication from occurring. Aspirin has been in use for a long time for various health conditions and is available as an over- the-counter medicine. Its role in Covid-19 is to inhibit platelet aggregation which reduces the risk of blood clotting. It also reduces inflammation and treats headaches and pain.
Enoxaparin, Rivaroxaban and Heparin
Enoxaparin is used for the prevention of deep vein thrombosis and pulmonary embolism. Because of its action in preventing blood clots, it can help treat worsening Covid-19. Enoxaparin and heparin are given by injection. Rivaroxaban is an oral anti-clotting medication that your doctor may prescribe for use at home. Heparin is usually reserved for hospital use.


Ivermectin
As above, ivermectin is a blood thinner.
Herbs and Foods
It is important to note many foods are actually flagged up by doctors when you are on anticoagulant medication because of their powerful anticoagulant activity! This includes cayenne pepper, turmeric, cinnamon, ginger, garlic, ginkgo biloba, vitamin E and fish oils. Add plenty to your diet while dealing with an infection and, if you have no appetite, make infusions or soups with bone broth, spices and herbs to maintain your immune system.
5.
Many over-the-counter medicines and home remedies can relieve symptoms and help a person feel more comfortable, including cough mixtures, antihistamines, acetaminophen (paracetamol, Tylenol), and nasal sprays, mouthwashes, and other mucus-reducing agents.
Saline or sodium bicarbonate solutions are effective and easy to prepare. Alternatively, to get rid of mucus in your lungs, you can try inhaling steam with a tea towel over your head and essential oils like Olbas oil or eucalyptus oil. Cinnamon, ginger, and honey can help to relieve coughing – try a cinnamon and ginger infusion with hot water, cinnamon and freshly chopped ginger.
This is an opportunity to take a superior quality multivitamin and mineral to support the immune system, as well as some of the other supplements mentioned above, or refer to your local herbalist for help.
If you are feeling poorly and have no desire to eat, drink plenty of anti-inflammatory herbal infusions, as above, and get a family member or friend to make a nourishing chicken broth or soup, in time-honoured tradition, replete with the minerals and collagen from the chicken and the minerals, vitamins and other healing substances from the vegetables, herbs and spices. This will support your immune system, your respiratory system, your digestive system, and speed up the healing process.
Remember: Treat early with a variety of therapies
Treat early with a range of therapies chosen from each of the five areas suggested with the expertise of health professionals from around the world. The medications and therapies you choose will depend on availability in your area and your trusted health professional’s recommendations. Use what is local, affordable, and available to you. You don’t need to take all of them!
When do I need to go to the hospital with a Covid infection?
If you have difficulty breathing, shortness of breath, chest heaviness, or are experiencing a sudden worsening of your symptoms, including numbness, or tingling anywhere in the body, unexplained swellings or rashes, faintness, confusion or disorientation, or acute pain, go to the hospital.
Lastly, rest often
Remember: the vast majority of people recover from Covid-19. Treat early and get plenty of rest, sunshine, and fresh air to reduce your illness’s length and severity. The body carries out the repair processes when resting. Do not be in a hurry to resume your usual physical activities and social engagements – doing so may set your recovery back. Rather, allow yourself a full two weeks to recuperate. Contact your doctor if you have any questions or concerns.
How does the illness progress?
SARS-CoV-2 infections range in severity. Some people will have no symptoms, some will have mild symptoms and people with pre-existing health conditions may have more severe symptoms that require hospitalization. Whether you have a confirmed Covid-19 infection or not, don’t delay seeking advice from a medical professional. Early treatment is key to prevent severe Covid-19.
As a rule of thumb, covid infections do not progress beyond the cold and fluey stages. For some people, the infection may result in a longer stage of illness beyond a month, now denominated ‘long covid’. People in this category may experience a number of side effects including general incapacitating or semi-incapacitating fatigue, continued aches and pains, continued loss of taste and smell, headaches, chest pain, breathlessness, brain fog, hair loss, digestive symptoms etc.
It is possible that these people may have underlying diagnosed or undiagnosed illnesses of an inflammatory nature – so the extra inflammation of the covid virus just pushes them over the edge to a zone where their immune systems are overburdened and cannot recover quickly. This might include common inflammatory diseases like diabetes, rheumatoid and osteoarthritis, hypertension, atherosclerosis etc.
The suggested treatment options above and, under the guidance of a health professional of your choice, with more sustained and targeted use of common remedies like vitamins D, C, ivermectin, quercetin, zinc, propolis, nigella sativa, n- acetyl cysteine, aspirin and other remedies, may also help you progress out of this prolonged inflammatory stage of the illness.
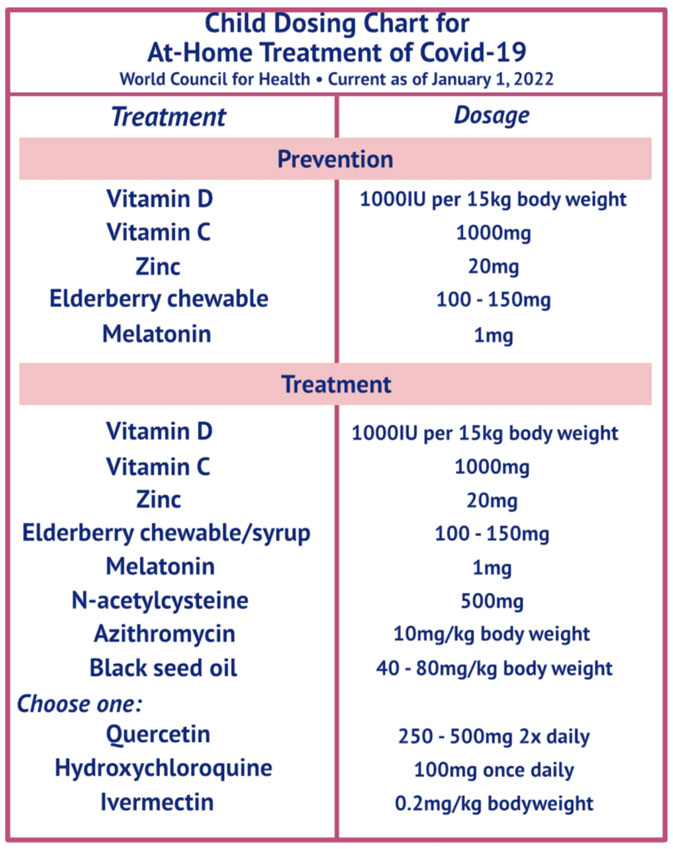
Adults should go to the hospital if they:
Children should go to the hospital if they:
are short of breath
are not interested in eating or breastfeeding
are light-headed (this can be a sign of decreased oxygen in your blood)
have a blue tinge to their lips
are having difficulty breathing
are confused
are experiencing chest heaviness or pain
have shortness of breath or difficulty breathing
have bluish lips
persistent fever or other symptoms for more than 7 days since onset
The coronavirus pandemic has had an enormous impact on physical and mental health across the world. Still, as we learn more about the illness, we can better treat and manage it so that severe illness is increasingly rare. The most important things you can do are to be prepared, take care of your immune system, and treat early using a combination of therapies that attack Covid from a variety of different angles.

This is an up-to-date guide to managing Covid-19 illness effectively at home. Covid should be treated early.
Maintain a healthy immune system with good nutrition, fresh air, and simple supplements like Vitamin D, C, Zinc, and Quercetin.
Use the medicines and supplements that are available to you.
Be prepared! Keep a good supply of healthy food, supplements, and medicines so you will be ready if you become infected.
Treat Covid-19 early if you become symptomatic or receive a positive test. Early treatment helps reduce the severity and duration of Covid-19 infection.
Treat Covid-19 using a combination of therapies that address the complex nature of the illness:
Antiviral/antimicrobial therapies such as ivermectin
Anti-inflammatory medicines such as ibuprofen and N-acetylcysteine
Immune-balancing medicines and supplements such as Vitamin D, Vitamin C, Zinc, Quercetin, and Melatonin
Anticoagulant medicines such as aspirin
Symptom support such as cough mixtures, acetaminophen, nasal sprays, and mouthwashes
Seek advice from your doctor if you are concerned about Covid-19 symptoms or for early treatment options.
GO TO THE HOSPITAL if you are short of breath, have difficulty breathing, or are experiencing chest heaviness or pain.
Take care to rest and resume normal activities slowly after a COVID-19 infection.
This list of medicines comprises over-the-counter (OTC) and prescription medicine for you to share with your doctor.
Be sure to read the patient information leaflet before using any OTC medicines to check whether they are suitable for you as an individual, especially if you are pregnant.
Aspirin and ibuprofen are not suitable for pregnant women, particularly in the last trimester of pregnancy. If your symptoms persist beyond 7 days, you feel your condition is worsening, your condition deteriorates suddenly, or if you are short of breath, contact your doctor or go to the emergency room.
If you need to go to see a doctor or go to the hospital, print this list of medicines out and take it with you.
Don’t forget:
The aim is to choose one treatment from the following categories: antiviral, anti- inflammatory, anticoagulant medicines (aspirin). Aspirin is the only anticoagulant to be safely used at home. In addition, choose several simple immune-supporting therapies, and other medicines that will make you more comfortable during infection.
The medications and therapies you choose will depend on availability in your area. Use what is affordable and available to you. You don’t need to take all of them!
Drink lots of water, take lots of rest, eat lots of fruit and vegetables, and get daily sunshine. Allow yourself at least two weeks to recover without strenuous activity. Do not expect to resume your usual exercise regimen and social engagements for at least two weeks. A positive attitude is essential!
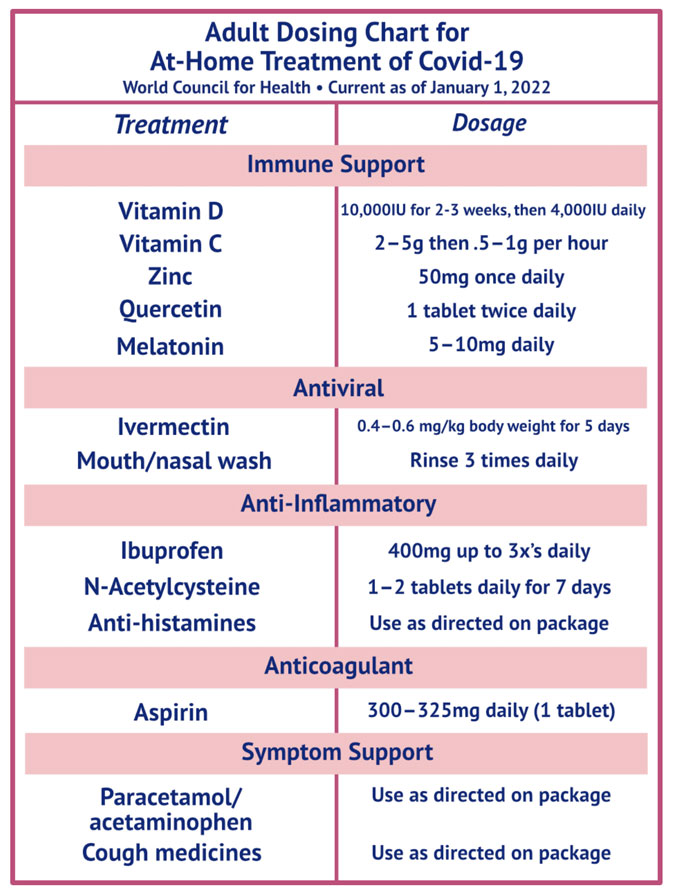
Immune Support Medicines
| Drug / Medicine | Recommended Dose |
|---|---|
| Zinc | 50mg once or twice daily |
| Vitamin D3 | 10,000IU for 2-3 weeks, then 4,000IU daily (2x dose: care home residents & people with highly melanated skin) |
| Vitamin C (ascorbic acid) | 2-5g, then 0.5-1g per hour |
| Vitamin B complex | 1 tablet daily |
| Vitamin A | 1 tablet daily |
| Quercetin | 1 tablet twice daily |
| Omega-3 fatty acids | 2-4g daily |
| Neem | 1 capsule once or twice daily, not for combination use with B-Complex supplements |
| Multivitamin | 1 tablet once or twice daily |
| Melatonin | 5-10mg daily |
| Lugol's lodine | 25mg daily as solution or tablets |
| Lactoferrin | 200mg twice daily |
| L-Lysine | 1000mg per day |
| Curcumin | 1 capsule once or twice daily |
| Black seed (Nigella sativa) | 1 capsule daily |
Immune Support Medicines
| Drug / Medicine | Recommended Dose |
|---|---|
| Antimicrobial mouth wash | Various OTC preparations, see below. |
| Antimicrobial nasal spray/rinse | Various OTC preparations, see below. |
| Azythromycin* | 500mg daily for 5 days |
| Colloidal silver | 5mls nebulised daily |
| Doxycycline* | 100mg tablet twice daily for 7 days |
| Hydroxychloroquine* | 200mg tablet twice daily for 5 to 7 days |
| Ivermectin* | 0.4-0.6mg/kg body weight for 5 days |
| Nitozoxanide | 500mg 2x daily after a meal for 5 days or until recovered |
| Artemisia | 1 capsule daily |
Anti-inflammatory Medicines
| Drug / Medicine | Dosage / Notes |
|---|---|
| Aspirin | 300-325mg (1 tablet) up to 4 times daily |
| Budesonide inhaler* | 800mcg – 1200mcg twice daily |
| Cetirizine | 10mg (1 tablet) daily |
| Colchicine* | 500mcg twice daily for 7 to 14 days |
| Corticosteroids* | Methylprednisolone, prednisone, prednisolone, dexamethasone, betamethasone; as prescribed |
| Cyproheptadine | 4-8mg 3 to 4 times daily, or as prescribed |
| Famotidine* | 20mg daily, or as prescribed |
| Ibuprofen | 400 mg up to 3 times daily |
| Loratadine | 10mg (1 tablet) daily |
| Montelukast* | 10mg daily for 14 days, or as prescribed |
| Naproxen* | 220mg (1 tablet) twice daily |
| Promethazine* | 10mg twice or three times daily |
| Drug / Medicine | Dosage/Notes |
|---|---|
| Aspirin | 300-325mg (1 tablet) daily |
| Riveroxaban* | As prescribed |
| Enoxaparin/Low molecular weight heparin* | As prescribed |
| Heparin* | As prescribed |
System support remedies for mucus
| Drug / Medicine | Dosage/Notes |
|---|---|
| Nebulised solutions | Various, e.g. sodium bicarb, colloidal silver nebulisation for 30 minutes 4 x daily |
| Bromexine | 8mg three times daily |
| N-acetylcysteine | 1 tablet (600mg) once or twice a day |
System support remedies for fever
| Drug / Medicine | Dosage/Notes |
|---|---|
| Acetominophen (Paracetamol, Tylenol) | 500mg up to four times daily |
System support remedies for cough
| Drug / Medicine | Dosage/Notes |
|---|---|
| Salbutamol syrup* | 1 teaspoon up to three times |
System support remedies for aches and pain
| Drug / Medicine | Dosage/Notes |
|---|---|
| Ibuprofen and aspirin | See ibuprofen and aspirin above (anti-inflammatory medicines) |
| Drug / Medicine | Dosage/Notes |
|---|---|
| Atorvostatin* | 40mg daily |
| Fluvoxamine* | 50mg daily or twice daily |
| Finasteride* | 5mg daily |
| Fenofibrate* | 160mg daily |
| Budesonide* | As prescribed |
| Decahedron* | As prescribed |
| Drug / Medicine | Equipment | To monitor oxygen saturation |
|---|---|---|
| To monitor oxygen saturation | Pulse oximeter | If less than 94%, go to hospital. |
| To check body temperature | Thermometer | 6 to 8-hourly or as needed |
| To relieve chest symptoms | Nebuliser | Four times daily with solutions as above |
| To relieve chest symptoms | Oxygen concentrator | For shortness of breath |
*By prescription only in most countries.
All listed therapies are given orally unless otherwise stated.
Ivermectin is also anti-inflammatory and immune-supporting. Similarly, several of the items listed under Immune Support also have anti-inflammatory and/or antiviral properties, e.g. neem and Lugol’s iodine.
Mouth and nasal hygiene solutions can be bought over-the-counter but a simple solution of sodium bicarbonate, salt, and purified water can be made at home.
The WCH Early Covid-19 Treatment Guidelines document and dosing charts are current as of Novembervembr 2022.
This article was reviewed by
Dr. Naseeba Kathrada, MD
Dr. Pierre Kory, M.D., M.P.A.
Dr. Tess Lawrie, MD, PhD
Dr. Peter A. McCullough, MD, MPH
This work is licensed under a Creative Commons Attribution 4.0 International License and is available for republishing and use as a Free Cultural Work.

Welcome to our new website, We have new content being added all the time, Sign up to receive regular updates.
Gmail has blocked our newsletter send.
Please use a different email address if possible.